Sophia McCarthy
Operations Manager
Did you know that the uterus can come in lots of different shapes and sizes? If an ultrasound reveals that your uterus is what we call an “abnormal shape”, it’s totally natural to feel a bit panicked. This certainly isn’t helped by the fact that even one innocent internet search for more details can produce an onslaught of alarmist headlines; unnecessarily scaring expectant mothers or those trying to conceive. We therefore felt it was important to clearly and calmly provide you with the facts surrounding these different shapes, as well as certain things you will need to keep in mind going forward.
What are the different kinds of uterus shape?
So, let’s start by differentiating between what uterus shapes are medically classed as “normal” and “abnormal”. As you read this list, please do note that while the word “abnormal” can sometimes have negative connotations, in this context, the classification is simply used to flag a difference – not to cause alarm.
Normal
Anteverted/Anteflexed Uterus
An anteverted or anteflexed uterus is the most common shape of the uterus. This means that the womb tilts forwards, towards your tummy.
Tilted / Retroverted Uterus
It is also common to have a tilted uterus, meaning the womb leans backwards towards your spine. A tilted uterus does not affect the shape of the uterus or its ability to function properly, and is therefore not considered an abnormality. While it can sometimes indicate other conditions that could affect fertility – such as endometriosis – a tilted uterus does not cause fertility issues or pregnancy complications.
Arcuate Uterus
An arcuate uterus is when there is a slight dip or indentation at the top of the womb. Similarly to a tilted uterus, an arcuate uterus shouldn’t affect fertility or cause pregnancy complications.
Abnormal Uterus Shapes
If your sonographer identifies any of the below shapes, please understand that an abnormal uterus is a congenital abnormality, meaning you were born with it. There is no way to prevent or stop the way a uterus forms – these anomalies just happen. In fact, according to babycentre.co.uk: “studies suggest that one in eighteen women can have a uterine abnormality”. Our experienced sonographers are well versed in identifying each type, and will know exactly how to monitor and support you throughout your fertility and pregnancy journey.
Bicornuate Uterus
One of the most common types of uterine irregularities is a bicornuate uterus: a uterus that has formed in a heart shape with an indentation at the top, creating two ‘horns’. This means there are two wombs that are connected to a single cervix. Below is a fascinating ultrasound image of a partial bicornuate pregnancy with lines indicating the separation. We can see that baby is growing in the left horn of the uterus!
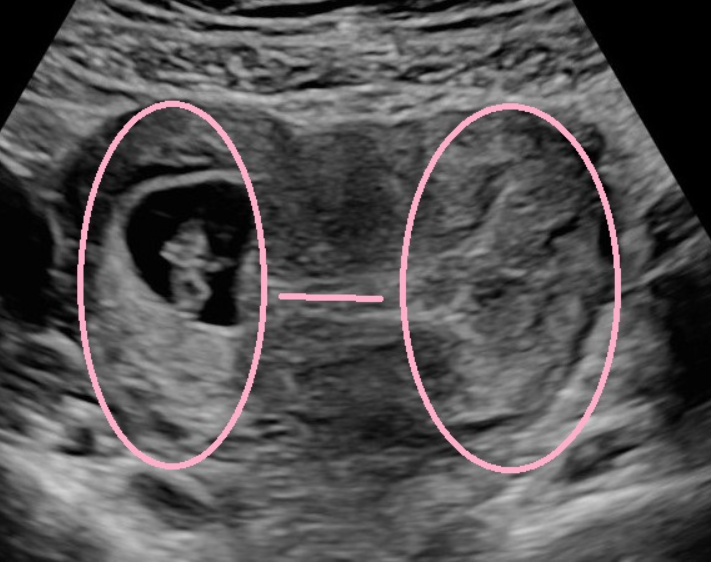
Risks: While a bicornuate uterus should not have an effect on fertility, there is a slightly increased risk of miscarriage and pregnancy complications, such as early delivery. You will therefore be monitored closely throughout your pregnancy to check the baby’s position.
Septate Uterus
Considered the most common abnormal shape (healthline.com), a septate uterus is when a layer of muscle divides the womb in two, right down the middle. This division can sometimes be partial (subseptate) if the division does not come all the way down.
Risks: A septate uterus may cause fertility complications. There is an increased risk of early term miscarraige and preterm birth. The baby may also be in an awkward position in the later stages of pregnancy.
Uterus Didelphys
Uterus Didelphys is an uncommon abnormality where the patient has two wombs, each with their own cervix and possibly a double vagina.
Risks: Uterus didelphys should not affect fertility. However, this abnormality has been linked to pregnancy complications and preterm labour.
Unicornuate Uterus
This is a rare abnormality where the size of the uterus is halved. There is only one fallopian tube. If a bicornuate uterus has ‘two horns’, a unicornuate uterus has ‘one horn’.
Risks: A unicornuate uterus should not cause fertility complications, however it does carry an increased risk of pregnancy complications and miscarriage.
These abnormalities are often visible during an Early Pregnancy Scan. They can also be spotted during a Pelvic Scan (please note, medical scans must be requested by your GP via referral).
If you would like more information on anything covered in this post, you can get in touch via info@theultrasoundsuite.ie or send us a message on our Facebook page and we will get back to you as soon as possible. Our website www.theultrasoundsuite.ie also provides a wealth of information on our various policies and procedures.
We look forward to seeing you soon!
Resources Used:
https://www.healthline.com/health/septate-uterus
https://www.verywellfamily.com/abnormal-uterus-and-miscarriage-risk-2371694
https://www.healthline.com/health/womens-health/bicornuate-uterus